

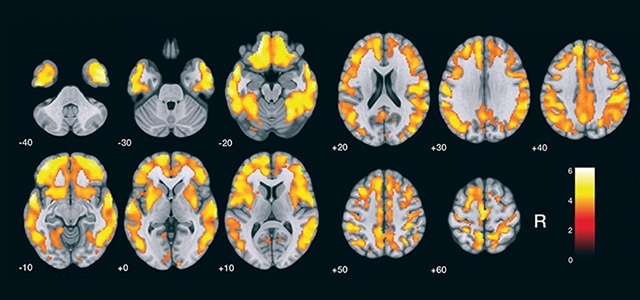
The nuclear medicine technique, combined with other kinds of analyses, more precisely distinguishes Alzheimer’s from other neurodegenerative diseases; the test has yet to be approved for routine use in clinical practice (image: Brazilian Journal of Psychiatry)
Published on 05/12/2021
By Maria Fernanda Ziegler | Agência FAPESP – Researchers in Brazil have validated a method for mapping the accumulation of amyloid-beta peptide in the brain using positron emission tomography (PET). In patients with Alzheimer’s disease, abnormal levels of this peptide clump together to form hard plaques in the cerebral cortex.
PET imaging, in conjunction with other kinds of analyses, is an important tool to help distinguish Alzheimer’s from other degenerative dementias. The new method has been tested in volunteers but has not yet been approved for routine use in clinical practice.
In the study, which resulted from a Thematic Project supported by FAPESP, the researchers validated a method for producing carbon-11-labeled Pittsburgh compound B (11C-PIB) and used it to map brain amyloidosis. The radiopharmaceutical was developed at the University of Pittsburgh in the United States and is widely used to perform noninvasive in vivo neuroimaging studies using PET scans. However, 11C-PIB, which is used in the technique as a marker of cerebral amyloid deposition, is not linked to any patent, aside from being hard to purchase on the open market, especially because of the very short half-life of carbon-11.
“During the research project, we were able to produce the radiopharmaceutical in Brazil, since it was already used by major research centers abroad. We validated the methodology and performed preclinical trials in animals. The method was then used in trials involving volunteer patients,” said Professor Geraldo Busatto Filho, head of the Psychiatric Neuroimaging Laboratory (LIM21) at Hospital das Clínicas (HC), the teaching and general hospital of the University of São Paulo’s Medical School (FM-USP), and principal investigator for the Thematic Project.
Alzheimer’s is the most common neurodegenerative disease in older adults, accounting for approximately 70% of all dementia cases. The diagnosis of Alzheimer's is still complex, often late, and achieved by the exclusion of other causes of dementia. This is because the neurodegenerative processes that characterize the disease begin years before the earliest symptoms, such as memory loss, difficulty participating in conversation or problem solving.
According to the researchers, the validation of markers such as 11C-PIB will contribute to earlier and more accurate diagnosis, as well as provide a new perspective on the disease so that novel treatments can be tested in future.
Worth a thousand words
After validating the brain amyloidosis detection methodology in Brazil, the researchers used statistical parametric mapping software to compare mean amyloidosis levels in 17 volunteers with Alzheimer’s, who were approximately 75 years old, to those of 19 healthy volunteers of a similar age (control). The validation process and test results are described in an article published in the Brazilian Journal of Psychiatry.
“From the statistical maps it’s easy to identify the accumulation of amyloid plaques in the group of patients with Alzheimer’s compared to the healthy volunteers in the control group. The cortical regions are clearly different. The statistical maps are pictures worth a thousand words,” Busatto said.
The Thematic Project was conducted at FM-USP. In addition to LIM21, it involved groups at the Center for Nuclear Medicine, headed by Professor Carlos Alberto Buchpiguel; the Cognitive and Behavioral Neurology Unit, led by Professor Ricardo Nitrini; and the Old Age Psychiatry Outpatient Clinic at the Neuroscience Laboratory (LIM27), headed by Orestes Forlenz.
Timing
Like the production of the radiopharmaceutical, 11C-PIB PET imaging of elderly patients with Alzheimer’s is no easy task since carbon-11 has a half-life of only 20 minutes. The isotope binds to amyloid plaques and emits gamma rays that are detected by the PET scan.
In the study with volunteers, the PET scanner and the cyclotron used to produce the isotope were in the same building as the machine that produced 11C-PIB, which was personalized for each volunteer.
“The radiopharmaceutical is injected intravenously and acts as a marker, binding temporarily to the amyloid protein clustered in the cerebral cortex, and eventually disappearing completely,” Buchpiguel said. “PET imaging via gamma rays displays the amyloid plaques in the patient’s brain in 3D. But you must have the requisite logistics in place to enable the scan to be performed before the radiopharmaceutical disappears.”
The researchers are conducting another study to compare the results in 120 individuals divided into three groups: patients diagnosed with Alzheimer’s, healthy older adults, and older adults with mild cognitive impairment.
Multiple tests
It is worth noting that brain mapping with 11C-PIB is not sufficient to diagnose Alzheimer’s or even indicate its severity. It serves only to distinguish Alzheimer’s from other forms of dementia.
“If the scan produces a positive result [showing brain amyloidosis] for a healthy individual, they won’t necessarily be diagnosed as having Alzheimer’s. The symptoms must be evaluated in association with the scan,” said Daniele de Paula Faria, a researcher at HC’s Nuclear Medicine Laboratory (LIM43) and a coleader of the study.
According to Busatto, validation of the method in Brazil coincides with a key moment in this area of neuroscience worldwide, placing the research group at FM-USP in an advantageous position to perform studies on Alzheimer’s.
“Clinical criteria for diagnosing Alzheimer’s disease dementia were revised in 2018 by the US National Institute of Aging and the Alzheimer's Association, which also issued new research guidelines for characterizing stages of the disease,” Busatto said. “It’s no longer diagnosed solely on the basis of a set of symptoms and signs of dementia. Typical pathological brain alterations also have to be detected, either by postmortem scanning of the patient’s brain or using new biomarkers while the patient is alive.”
The PET scan to detect brain amyloidosis provides one of these biomarkers, he added. Indeed, with the revised criteria, it is one of the most important diagnostic methods. “In countries with access to the technology, the test has been associated with clinical and neuropsychological criteria used to identify symptoms of dementia and cognitive deficits. A combination of multiple tests is needed to confirm a diagnostic hypothesis of Alzheimer’s and rule out other causes of dementia,” Busatto said.
Diagnoses based only on symptoms turn out to be wrong in at least 30% of cases. “However, studies show that if we offer this type of test at a memory clinic, the diagnosis will change for some patients. This could be most important in terms of public health in future,” Busatto said.
Multimodal protocol
In the Thematic Project, the research group also deployed PET scans with the biomarker fluorodeoxyglucose (FDG). This radiopharmaceutical, which contains the isotope 18fluorine (18F-FDG), is used to map the brain’s glucose metabolism. Unlike the isotope used to detect amyloid plaques, this one acts as a marker of neural activity.
These scans were approved many years ago and serve to reinforce the diagnosis of Alzheimer’s. “It can verify brain damage evolution and severity in Alzheimer’s. It also helps distinguish Alzheimer’s from other forms of dementia,” Buchpiguel said.
A typical sign of neural damage due to Alzheimer’s, he added, is loss of brain cells’ capacity to metabolize glucose, reflecting a decline in their functional activity. “Imaging with 18F-FDG identifies brain regions in which levels of the isotope are altered, showing that neurons have stopped working or become less active even though they’re still present,” he explained.
11C-PIB PET imaging to map brain amyloidosis detects neuropathological alterations considered characteristic of Alzheimer’s, and according to the researchers, it can be used for the early detection of amyloid plaque deposition.
The glucose metabolism scans (18F-FDG) map the neurodegenerative alterations that typically signal the onset of cognitive impairment. The more the symptoms progress, the greater the glucose metabolism deficit in the brain regions damaged by Alzheimer’s.
In the study performed for the Thematic Project, each volunteer underwent an MRI scan, as well as PET scans to map brain amyloidosis (11C-PIB) and glucose metabolism (18F-FDG). This procedure enabled the group to create one of the first and most comprehensive databases in Latin America for older adults examined with neuroimaging markers and recruited by the same research center.
“Besides clinical and cognitive assessments, the database reflects what we call a multimodal neuroimaging protocol, as we performed MRI and PET scans on all three groups,” Busatto said. “We’ve obtained a range of data that enables us to make several comparisons of brain structure and functioning. We still have a great deal of work to do.”
The multimodal protocol, executed in partnership with HC’s Neuroradiology Laboratory (LIM44), is designed to measure the volume of different brain regions, look for small vascular lesions, examine white matter integrity, and analyze functional connectivity (how the brain is organized in terms of major networks).
“We’re making correlations among markers, clinical data and brain images in the same patients involved in the study. Identifying complementary or correlated markers can help us discover the extent to which patients with cognitive impairment could potentially develop Alzheimer’s, as well as offering information on the stages through which the disease progresses,” Buchpiguel said.
Source: https://agencia.fapesp.br/30728