

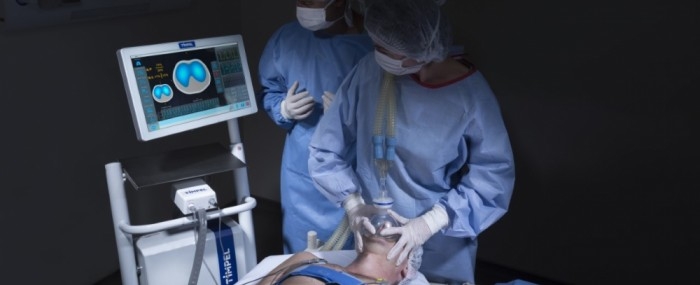
An electrical impedance tomography system was developed by a São Paulo-based startup to monitor the lungs of patients on mechanical ventilation uninterruptedly and noninvasively (photo: Timpel)
Published on 03/18/2021
By Elton Alisson and Eduardo Geraque | FAPESP Innovative R&D – A mechanical ventilation monitoring system using electrical impedance tomography (EIT) developed by Timpel, a startup based on São Paulo, Brazil, is being used in several countries to provide intensive care for critical patients with COVID-19. Developed with support from FAPESP via its Innovative Research in Small Business (PIPE) Program, the system provides vital real-time information for medical teams at the bedside to monitor the patient’s lungs uninterruptedly and noninvasively. This optimizes mechanical ventilation, reducing the amount of time during which patients depend on the machine to breathe and minimizing the adverse side effects of intubation.
The system was originally designed to monitor all patients who needed mechanical ventilation in intensive care units (ICUs), regardless of the disease. With the emergence of the coronavirus pandemic, researchers at Timpel began adapting the technology to help medical teams treat critical COVID-19 patients.
In this venture, they were supported by funding awarded to a project selected in a call for proposals issued by PIPE-FAPESP in partnership with FINEP, the Brazilian government’s innovation agency, to foster the development of products, services or processes by tech startups and small businesses in the state of São Paulo to combat COVID-19.
“We want to use the knowledge accumulated by physicians who have treated COVID-19 patients in European countries such as Italy and Spain, where the contagion curve has peaked, and in the United States and Brazil, where it continues to rise, to upgrade our system so that it can be used in a more personalized and intuitive manner,” said Timpel CEO Rafael Holzhacker.
The technological principle behind EIT is resistance to electric current flow (impedance) in the lungs, which varies considerably as the patient breathes in and out.
A weak electric current is passed through a chest belt with 32 electrodes (similar to those used to produce an electrocardiogram) and highlights the region in which air meets differences in resistance as it is circulating. On the basis of the impedance measured on the surface of the patient’s chest, 50 images are generated per second, showing the distribution and dynamics of lung insufflation and supplying the doctor at the bedside with vital real-time information.
Onboard software developed during the PIPE-supported project enables the medical team to assess the ventilation strategy that bests protects the patient.
“The system lets the team evaluate the patient’s progress from the bedside, reducing the need for CT scans, exposure to radiation and the risk of transfer to the radiology suite, which is especially hazardous for COVID-19 patients, who must be kept in isolation,” Holzhacker said.
Several innovations
Through the project supported by PIPE-FAPESP, the researchers now plan to simplify the onboard software to reduce the cost of the machine and to enable medical teams to operate the system remotely so they can avoid having to circulate a great deal in ICUs. “This will also allow the staff of reference hospitals to assist hospitals located in places distant from major cities and with scant human resources,” Holzhacker said.
Belts and electrodes that come into contact with the patient’s skin will be disposable, in contrast with those regularly used in tomography. “The device will be configured to run on battery power, which could be crucial during patient transfer and in remote areas of Brazil,” he said.
Another innovation, he added, will be the development of an entirely novel application for use in monitoring mechanical ventilation that will be programmed to recognize the clinical characteristics that are being observed in cases of COVID-19.
“All these innovations are intended to make life easier for medical teams,” Holzhacker said. Studies of COVID-19 cases and the clinical experience of physicians involved in the treatment of patients with the disease show that mechanical ventilation in ICUs must be adjusted to the individual needs of each patient to minimize the adverse events it can cause.
“Our system is affordable for public as well as private hospitals and will help keep up with demand, which unfortunately, will remain high for a long time,” Holzhacker said.
More than 150 units of Timpel’s EIT system are currently in service in the US, Italy, Spain and elsewhere. In Brazil the system is used by the Heart Institute (INCOR) of the University of São Paulo’s Medical School (FM-USP) and by Hospital das Clínicas, the general and teaching hospital run by FM-USP, as well as Emílio Ribas Institute (IEER), a major infectious disease hospital also located in São Paulo, and several private hospitals.
Timpel was initially incubated at the Center for Innovation, Entrepreneurship and Technology (CIETEC), run jointly by the University of São Paulo and the Nuclear and Energy Research Institute (IPEN).
To produce the first units of its system, the firm partnered with University of São Paulo’s Medical and Engineering Schools and the Federal University of the ABC (UFABC). They were first sold in 2015, after approval was won from ANVISA, Brazil’s national health surveillance agency, as well as from the European Union, and the US Food and Drug Administration (FDA).
The firm has a branch in the Netherlands.
Source: https://agencia.fapesp.br/33986