

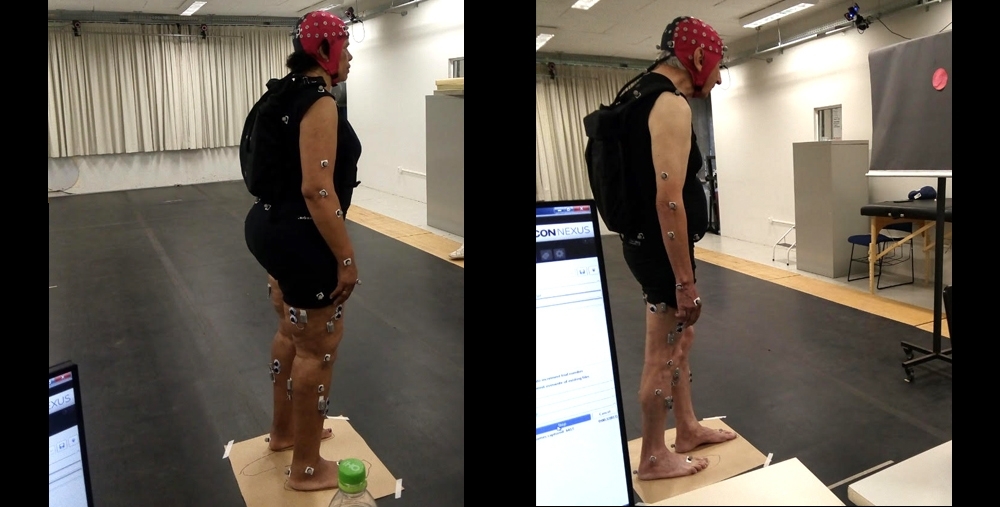
Researchers at São Paulo State University described in detail the positive effects of levodopa on posture and balance, in a study aimed at optimizing treatment. The findings are reported in Brain Research (photos: Fabio Barbieri/MOVI-LAB)
Published on 11/07/2022
By Karina Ninni | Agência FAPESP – Scientists at São Paulo State University's Human Movement Research Laboratory (MOVI-LAB) in Bauru, Brazil, have succeeded in measuring the impact of the drug levodopa on postural and balance control in patients with Parkinson’s disease. They also determined that the positive effects of the drug begin about 60 minutes after ingestion and last for about another 60 minutes.
They expect their findings, reported in an article published in Brain Research, to help optimize treatment of the disease. They were supported by FAPESP via two projects (17/19516-8 and 18/03448-6).
Considered essential in treating Parkinson’s, levodopa increases the amount of dopamine in the brain, which reduces the symptoms of the disease. In the study, the researchers monitored 15 mild to moderate patients after they took the first dose of the day. They had all been using levodopa for more than six months; many also used other drugs.
“We worked with patients in stages 1 to 3 of the disease [on a scale from 1 to 5]. Patients in these stages, which are mild to moderate, exhibit initial changes in posture and balance but haven’t yet lost their independence. Most studies focus on these stages because the aim is to improve treatment quality,” said Fabio Augusto Barbieri, a professor in UNESP’s Department of Physical Education and its Graduate Program in Human Movement Science.
The group opted to study the effects of the first daily dose of the drug because there tend to be fewer fluctuations in the time taken for its effects to begin and their duration. “Even so, they vary from patient to patient. The effects of the first dose are nonetheless more regular,” Barbieri said, adding that the number of doses taken by each patient depends on the stage of the disease, among other factors.
Two aspects of the research should be highlighted, Barbieri continued. “The study advances by determining a suitable period for assessment of postural and balance control: a standard period for other studies to gauge the effects of the drug, and also for treatment, since if physicians know how long the drug’s effects on balance last, they can prescribe an ‘ideal’ period for physical exercise and improve the efficacy of the intervention,” he said. “However, it's important to bear in mind that our findings in this study are valid only for postural and balance control, on which it focused. For gait and upper limb control, for example, the ‘window’ may have to be a little different.”
Cortical effect
Barbieri noted that the experiment set the patients a demanding postural task. “They were asked to stand still for a minute in bare feet, with one foot in front of the other and arms relaxed beside their body, looking at a static point about 1 m away. They repeated this task three times,” he said. “In other studies, their feet were side by side and no positive effects of levodopa were detected, but the postural task was much easier. Previous research corroborates this hypothesis of positive effects in more challenging tasks.”
The volunteers visited MOVI-LAB twice, with an interval of at least seven and at most 14 days. In both cases, they came to the lab at least 12 hours after the last dose and were assessed before and after taking the drug (which the authors call off- and on-medication respectively).
The patients were assessed every 30 minutes for three hours after their first morning dose. Clinical variables were measured on one of the visits and postural control on the other.
The scientists measured variations in the patient’s center of pressure (CoP) using a force platform. They also measured muscle activity with an electromyograph and cortical activity with electroencephalography (EEG), a procedure that records spontaneous electrical activity in the different regions of the cortex.
“We measured CoP, muscle activity and cortical activity at different times after the patients took levodopa,” Barbieri said. “When we compared the results, we detected an increase in electrical activity 60 minutes after the drug was taken, showing that the cortical regions of interest were more active and the patient was better able to deal with the effects of the disease on the brain in terms of postural control. The patient produced a more adequate motor signal for better control of posture.”
All the signals measured (CoP, muscle activity and cortical activity) were electronically synchronized and analyzed using Matlab, a high-performance numeric computing platform. “As far as we know, this is the first investigation of the dynamics of postural control [via cortical activity, muscle activity and body movement] in response to levodopa while performing a challenging standing task,” Barbieri said.
Windows
Because treatment of the disease includes exercise, the results of the study can help physicians prescribe motor interventions. “If we want treatment to have a better effect on postural control, exercise should be performed in the window between 60 and 120 minutes after the first dose in order to ensure that the patient gets the best possible result,” Barbieri said, adding that the group did not expect the effects of the drug to last as long as two hours. Other studies had already established the 60-minute threshold.
The next step, according to Barbieri, entails proposing interventions that improve postural control and balance. This means combining the drug with exercise and determining the most suitable period for the exercise training. “We’ve seen studies in the literature that combine various types of rehabilitation in an endeavor to slow progression, including medication, exercise training, speech therapy and physical therapy, among others,” he said. “If the intervention is done with optimal timing, progression of the disease can be braked even more. However, more research is needed to establish the best time to intervene. That's the context for our work.”
Early onset Parkinson’s
Most Parkinson's patients are idiopathic, meaning the cause is unknown. Idiopathic Parkinson’s manifests mainly as postural instability with gait dysfunction, or as resting tremor. “To date, we have found out that the disease can be caused by genetic factors, environmental exposure, lifestyle [unhealthy habits, diet, sedentarism], toxic substances in the workplace, neural lesions and even drug abuse,” Barbieri said.
The typical patient profile has changed. “We used to see disease only in older people, especially the over-60s, but there are more and more cases of early-onset Parkinson’s, where the patient is under 50,” he said. “It could be because technological advances are making earlier diagnosis more frequent. The disease has been publicized and gained more visibility in recent years. These factors apparently affect the age at which the disease is diagnosed, and patient characterization is improving as a result.”
The article “Temporal dynamics of cortical activity and postural control in response to the first levodopa dose of the day in people with Parkinson’s disease” is at: www.sciencedirect.com/science/article/abs/pii/S0006899321005849.
Source: https://agencia.fapesp.br/40006